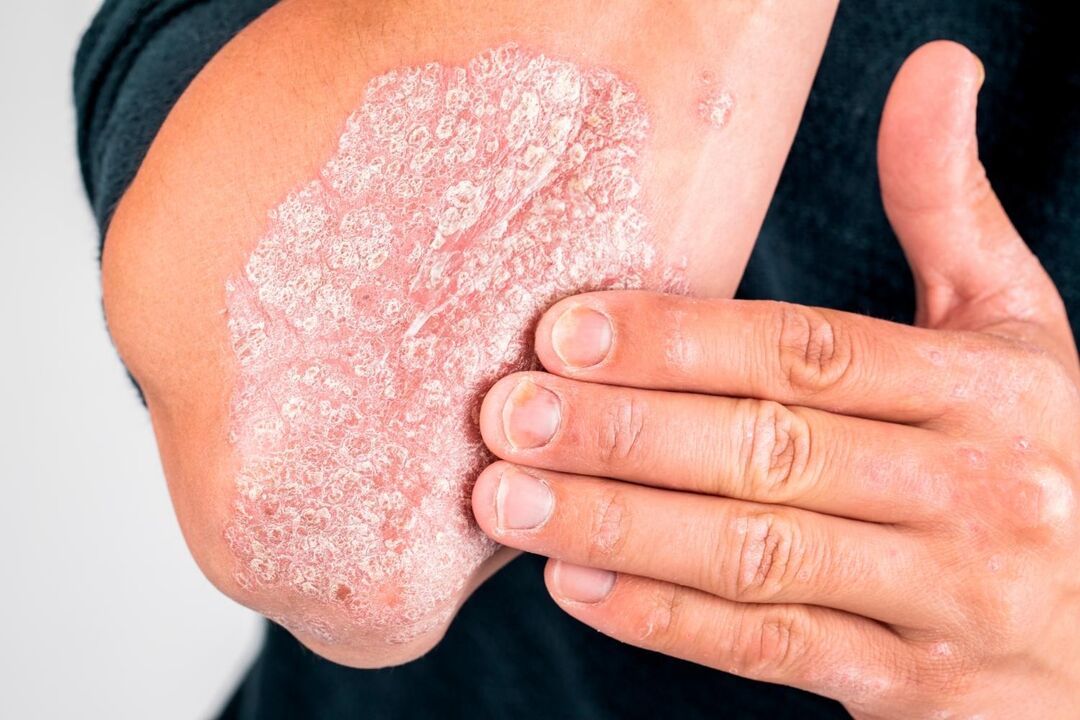
A pathological condition characterized by scaly and nodular changes of the skin and nails is called psoriasis. Dermatologists are involved in the diagnosis and treatment of the disease.
Psoriasis is a chronic skin and nail disease in which a rash of pink nodules and silvery scales appears on the skin. Usually the nodules merge into large plaques, around which the skin is rapidly covered with scales. With prolonged development of the disease, joint damage is possible, accompanied by impaired mobility and constant pain. Different forms of psoriasis differ in the degree of skin damage: the patient may have only thin spots on the scalp or large plaques on different parts of the body. The likelihood of developing complications of psoriasis also depends on many factors. This disease is especially dangerous for pregnant women, since the pustular form of the disease can cause miscarriage.
About the disease
Psoriasis is one of the most common skin diseases. The first symptoms of skin changes usually occur between the ages of 18 and 35. Often psoriasis occurs against the background of cardiovascular disorders, Crohn's disease and depression. About 30% of patients develop joint damage (arthritis). It is impossible to eliminate the root cause of psoriasis, however, symptomatic therapy can significantly alleviate the course of the disease.
Types of psoriasis
Depending on the prevailing symptoms, several types of psoriasis are distinguished:
- plaque: characterized by the appearance of classic plaques covered with silvery scales; preferred location: elbows, knees, torso, scalp;
- teardrop-shaped - the main manifestation is pink-orange nodule nodules ranging in size from 1 to 10 mm;
- nail psoriasis: the nails are predominantly affected;
- large fold psoriasis - rashes occur in the armpits, in the folds of the neck, on the genitals and other places with excessive friction; this form is more common in obese people;
- head psoriasis - the scalp is affected;
- arthropathic psoriasis (psoriatic arthritis): the joints are affected;
- pustular psoriasis - multiple small blisters with pus appear on the patient's skin;
- psoriatic erythroderma - in addition to the rash, there is a pronounced reddening of the skin in the area of the rash.
Symptoms of psoriasis
Most often, plaques appear on the forearm, lower leg, navel and scalp. The pustular form of psoriasis is characterized by the formation of pus-filled blisters on the skin. At certain times, many patients experience a change in the color and texture of their nails. Damage to the skin scales leads to the appearance of pinpoint bleeding. Patients also complain of itchy skin. Skin changes periodically disappear and reappear.
Other symptoms and signs:
- the appearance of red spots in the area of \u200b\u200bthe skin folds;
- profuse rashes occur after infectious diseases and stress;
- slight increase in body temperature;
- the appearance of new rashes in the winter months;
- articolar pains;
- reduced mobility in the affected joint area;
- dryness and hypersensitivity of the skin.
Resorption of plaques usually begins from the central part, as a result of which the psoriatic elements acquire a ring-like or garland-like shape. Temporary depigmentation (pseudo leucoderma) remains at the sites of resolved rashes. During periods of incomplete remission, single "service" plaques may remain in some areas of the skin (most often in the area of \u200b\u200bthe elbow and knee joints).
The most severe types of psoriasis are psoriatic erythroderma and arthropathic psoriasis.
In psoriatic erythroderma, the entire (or almost all) skin is involved in the pathological process. The skin becomes taut, rough, infiltrated, red in color, with abundant flaking with large and small lamellae on the surface. Peripheral lymph nodes increase, subfebrile temperature appears, the general condition of patients is disturbed, changes in blood (leukocytosis, elevated ESR), urine (proteinuria) are observed. The development of erythroderma is promoted by irrational and irritating therapy in the progressive stage of psoriasis.
Arthropathic psoriasis is characterized by lesions predominantly of the small joints of the hands and feet, less often the wrist, ankle, intervertebral, etc. , accompanied by severe pain and swelling of the joints, limitation of their mobility and deformity. Radiography reveals lysis of the distal phalanges of the fingers and changes in the joints, similar to rheumatoid arthritis. The Waaler-Rose test and latex test are usually negative. In the blood, leukocytosis, elevated ESR, hypergammaglobulinemia. Joint involvement may be associated with skin lesions or be isolated over a number of years.
With all these forms of psoriasis, it is possible to damage the nails in the form of perforated nail plates ("thimble phenomenon"), their dullness or thickening up to onychogryphosis. The course of the disease is chronic and wavy. The seasonality of the process is usually expressed - deterioration in winter with a significant improvement in summer (winter type), less often - vice versa (summer type).
Causes of psoriasis
The exact mechanisms of psoriasis formation are not yet understood. It is thought to be an autoimmune disease in which the body's defense system mistakenly attacks healthy tissue. The T cells and neutrophils needed to fight off pathogens can begin attacking skin cells and joint structures. In this case, characteristic skin changes occur, including the formation of bubbles with an inflammatory fluid. The expansion of blood vessels in the area of \u200b\u200bthe inflammation is accompanied by redness of the skin. Autoimmune disease can be caused by hereditary factors.
Additional risk factors:
- skin infections. First of all, these are bacterial infections caused by streptococcus;
- skin damage from cuts and burns;
- prolonged stress and psychotraumatic factors;
- alcoholism and smoking;
- vitamin D deficiency in the body;
- taking certain medicines, including lithium and beta-blockers;
- unfavorable family history. The discovery of psoriasis in a close relative of the patient indicates the possibility of a genetic predisposition to this disease;
- acquired or congenital immune impairment. It could be an HIV infection, AIDS, or another condition.
Despite the discovery of the presumed immunopathological causes of psoriasis, the disease remains poorly understood. There are a number of diseases and lifestyle features that cause the manifestation of hidden predisposing factors for this disease.
Psoriasis diagnosis
If skin changes appear, you should consult a dermatologist. The doctor of our clinic first performs a general skin examination to assess the nature of the rash. Soft scraping allows you to detect peeling papules and a thin film under the nodules. Under the film is a moist skin surface, prone to small bleeding. At the same time, there are atypical signs of psoriasis resembling other diseases, so the doctor must conduct instrumental and laboratory diagnostics.
- Blood analysis. The dermatologist prescribes a venous blood test to rule out other diseases and detect signs of psoriasis. In the treatment room, the nurse treats the skin of the patient's cubital fossa with an antiseptic, applies a tourniquet and draws blood with a syringe. In our laboratory, specialists first rule out the presence of rheumatoid factors. In pustular psoriasis, an increased rate of erythrocyte sedimentation is often found. Elevated uric acid levels are detected;
- Examination of pustule fluid. The doctor collects the liquid in a sterile container and sends the material to the laboratory. Microbiological examination does not reveal a bacterial culture, but there is an increase in the number of neutrophils characteristic of psoriasis;
- Skin biopsy. The dermatologist prescribes this study to make an accurate diagnosis for atypical skin rashes. During the procedure, your doctor treats your skin with an antiseptic, numbs it, and removes a small area of skin with a scalpel. The tissue material is studied in the laboratory of our clinic using microscopy. The results allow to clarify the cellular composition of the nodules;
- X-ray of the affected joint. The doctor orders this study to determine the type of arthritis. Also, in severe complications of arthropathic psoriasis, X-ray diagnostics of bones is required;
- Scrape the skin to rule out fungus. The doctor cleanses the skin surface and, using a special spatula, collects several scales for microbiological examination. This analysis is mainly needed if the rashes occur only in the area of \u200b\u200bthe foot and nails.
If necessary, a consultation with a rheumatologist is carried out.
Expert opinion
Psoriasis is a disease with many manifestations. It can be nearly invisible or cause serious health problems. The most dangerous complications of psoriasis are joint damage, which can cause disability in the patient. Also, the disease can lead to autoimmune disorders, especially Crohn's disease and ulcerative colitis, metabolic pathology, erectile dysfunction in men. Women suffering from psoriasis can experience infertility and miscarriage. To prevent these complications, it is necessary to consult a doctor immediately after the appearance of suspicious signs, and with an already diagnosed diagnosis, carefully follow all the recommendations of a specialist.
Treatment of psoriasis
The main focus of the treatment of psoriasis is symptomatic therapy. Patients need drugs that reduce inflammation and prevent the formation of rashes. In addition to drug therapy, the dermatologist of our clinic necessarily prescribes a special diet for the patient. Normalizing your lifestyle and eliminating stressors can reduce the severity of your psoriasis symptoms.
Depending on the situation, a dermatologist can use different methods to treat the disease.
- Administration of corticosteroids. The dermatologist prescribes ointments containing these drugs. The beneficial effects of corticosteroids include reducing inflammation in the tissues and eliminating itching;
- Vitamin D supplements. Synthetic forms of this vitamin slow the growth of skin cells, thus preventing the formation of scales and nodules;
- Therapy with drugs containing vitamin A derivatives. A dermatologist prescribes retinoid ointments to reduce inflammation and itching. These medicines increase the skin's sensitivity to light, so sunscreen should be used;
- Use of calcineurin inhibitors. These are immunosuppressants that reduce inflammation. The dermatologist prescribes topical agents such as tacrolimus. Such drugs are used in a short course to prevent the development of side effects and complications;
- Skin treatment with salicylic acid to remove dead skin cells. A dermatologist prescribes this drug along with corticosteroids for complex skin treatment;
- Using a moisturizer to get rid of dry skin and itching;
- Irradiation of the skin with ultraviolet light. This safe physiotherapy treatment method improves the functioning of local immunity. The doctor selects an individual dose of radiation for the patient;
- Phototherapy. This method involves irradiation of the skin using special devices. Phototherapy combines the technologies of laser therapy and photochemotherapy;
- Joint puncture in severe psoriasis. The doctor treats the skin at the puncture site with an antiseptic, numbs the tissues and inserts a needle. With the help of a syringe, drugs are injected into the joint cavity to reduce the inflammatory process.
The dermatologist monitors all stages of treatment to achieve the best result and prevent complications. Corticosteroids, retinoids and calcineurin inhibitors are used strictly under the supervision of a specialist.
Prevention of psoriasis
The recommendations of the dermatologist of our clinic will help reduce the severity of rashes and alleviate the course of the disease.
Prevention of exacerbations of psoriasis:
- relieve anxiety and stress by improving sleep, avoiding coffee, and taking prescription sedatives;
- exclusion from the diet of foods containing allergens;
- timely treatment of infectious skin diseases.
Rehabilitation
Psoriasis is a chronic disease that cannot be cured. Rehabilitation measures are aimed at preventing relapses. Depending on the form of the disease, physiotherapy, spa treatment, mud therapy, therapeutic baths and other procedures may be prescribed.
Questions and answers
Is it possible to cure psoriasis with folk remedies?
There are no proven effective methods. It is important not to trust dubious types of treatment, but to follow the recommendations of the attending physician.
Does stress affect the course of psoriasis?
Yes, stressful situations can aggravate the course of the disease.
























